My C Section Experience
My Caesarian Experience
It wasn’t what we wanted, but it was a medical need, due to
my chronic high blood pressure turn severe preeclampsia (according to the
hospital discharge notice). We
could have opted for induction, but because it was so early in the pregnancy
(37weeks), Dr. Wild said it wasn’t a good environment to attempt induction
(i.e. my body and the baby weren’t ready for labor and if forced on either of
us, my blood pressure could spike or the baby could be put under duress). Those situations during induction would
then require an immediate emergency caesarian.
It was good that we did the scheduled c-section instead of
induction, because the baby was too high up into my ribs and the cord was wrapped
around his neck. But I’m getting
ahead of myself…
The surgery was scheduled for noon on Feb 18, 2013 at East
Jefferson General Hospital. The
night before, no food or water from midnight on. We arrived 2 hours (10 am) prior to surgery, as required by
the hospital. We walked into the
labor and delivery, and Greg said, “We’re here to have a baby. Literally.”
The nurses confirmed our names and walked us into the prep
room. It was large, plenty of
space and it’s where we stayed until the surgery was to take place. The nurse gave me the hospital gown to
put on and Greg put on his Daddy scrubs that I bought for him for Valentine’s
Day.
The baby monitor was put in place – basically it’s the NST
machine – two straps go around the belly, with one strap monitoring the baby’s
heart rate and the other monitoring any contractions. As typical, the nurse had a difficult time getting the
baby’s heart rate in place, because the baby was moving so much.
I have small veins and only once before needed an IV, which
was not a pleasant experience. I
looked at the nurse and said, “This is going to hurt, isn’t it?” She looked a little sad and nodded her
head, “Yes.” I closed my eyes and
she dug into my hand. She did
better than the IV I had years ago, but it did hurt. Why don’t they give a shot before having to dig for a vein? Because she had to dig, it was a bloody
mess on my left hand.
And then the chills came. With high blood pressure, they need to pump you full of
fluid, to keep the pressure at a constant during the surgery. For me, the fluid sent chills, the type
that I couldn’t stop my body from shaking and feeling an intense cold. I didn’t know if the shakes were from
being so nervous or not. Then I
realized that when the drip from the IV bag ended, I wasn’t shaking… and when
another IV bag was added, I started shaking again… I understood it was the
fluid causing the shakes.
Though we were reassured constantly that the surgery would
start on time, Dr. Wild didn’t show up until 12:30. I was almost expecting this, because I knew she had a
surgery earlier that morning and I imagine, nothing starts or ends on time when
one is in the hospital.
While we waited for Dr. Wild, the anesthesiologist doctor
came in to introduce himself as the one who would give me the spinal
epidural. Unlike the epidural given
during labor, the spinal epidural would be one shot and no tubes would be taped
to my back for additional pain relief (because they have a good approximation
of how long the surgery should last).
We also were introduced to two other assistants to the anesthesiologist
doctor.
Honestly, it was a little scary to meet three people who
would govern my critical life functions through surgery.
When Dr. Wild arrived, things went into motion fairly
quickly. I was wheeled into the
surgery room. My husband was not
allowed to be in the room while the anesthesiologist gave me the spinal
epidural, because the hospital requires sterilization for the process.
I was told to sit up on the hospital bed. A nurse stood in front of me and told
me to put my head (front of head, my face down to the ground) into her chest
and to curve my back in the worst possible posture (the kind your mom would
fuss at your for).
I felt the anesthesiologist clean my back three times with a
cold towel of sorts and then put that square paper in place on my back. He warned me of the burn before he did
so and yes, it did burn, like fire going into my body. And it wasn’t just a “ok, that’s the
shot.” It was the burn and then
“just a little more” – pressure and burn.
The nurse helped me lay back down on the table and the
tingling in my legs and feet started within seconds. I think I told the anesthesiologist, “I can feel my feet
tingling, as if my feet fell asleep, but I can feel it” at least four
times. I guess I didn’t want them
to start anything until I knew I couldn’t feel anything.
The blue sheet was put in front of my face and I heard Dr.
Wild say, “I see you waited for me.”
(Saying this, because we had a blood pressure scare a week prior to the
scheduled c-section and the doctor was out on vacation.)
Nurses explained that they were putting the catheter in,
fortunately the epidural was in full swing and I didn’t feel that.
Then I heard Dr. Wild ask the anesthesiologist, “How is her
blood pressure?” He made a face,
looked away from me and I heard Dr. Wild reply, “That happens when she’s
nervous.” So, I imagine the blood
pressure was high. I remember
thinking to myself, “I’m making my blood pressure spike with being nervous. Close your eyes and think calm
thoughts.” I don’t know if that
helped, but soon after, Dr. Wild said, “Alright, all we need now is the Daddy.”
It was a relief when I heard Greg’s voice. I was nervous, but he was there and it
would be OK. I knew when they
started, not because I felt pain, but because of all of the tugging. I felt as if someone was trying to pull
my body through a wall on the other side.
This lasted for a while, come to find out from some nurses, basically
the doctor has her hands and arms up into the body, moving organs, stomach etc
out of the way, because the baby was so high up (as into the ribs as he could
be).
(When we went to the prenatal classes, the instructor makes
it seem like the baby is right there at the incision point and the baby is
quickly born – this is typically not going to be the case!)
At various points, I have to admit that the anesthesiologist
assistants were really good, because they would ask how I was feeling. If I felt sick to my stomach, then they
did some type of adjustment and asked if I felt better, which helped. The nurses were very spot on with
caring for my needs during the surgery.
When Dr. Wild announced, “Do you have the camera ready? The baby is coming out.” Greg asked if he could video it and
there was a slight hush. Hospital
policy is “no videos.” But Dr.
Wild was really cool. She said,
“Go ahead, I have nothing to hide.”
If she hadn’t said that, I never would have been able to see our son
being born. At the beginning of
the video, you can actually see the doctor unwrapping the cord from around the
baby’s neck and then pulling him out by his head (which weirds a lot of people
out). It’s a bloody video, but
isn’t that life..
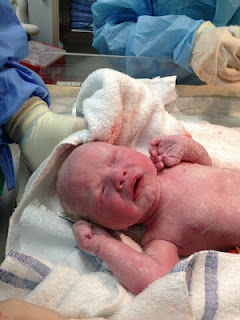
Gregory Patrick O’Brien Jr was born as 12:58pm on Feb 18th,
weighing 6 pounds 12 ounches and 20 inches long with a head full of blond hair
and grey/blue eyes.
On the other side of the blue sheet, I cried when I heard
our son’s cries. I knew he was
OK. I was waiting for his first
cries, to reassure myself that he was alive and well. It was a beautiful sound. The sweetest I’ve ever heard.
The nurses took the baby to the other side of the room. Greg watched as they wiped the baby
off, took his weight and footprints.
The nurse at my side moved the blue sheet to the side so I could watch
as our baby was weighed, etc. I
heard him crying and when Greg carried him to me and we took our first picture
as a family, Gregory stopped crying.
It was a magical moment.
One of the best experiences.
If I could stop the caesarian experience at this point, it
would be rainbows and unicorns, but it goes on…
My husband went with the baby to the nursery while Dr. Wild
finished up with the surgery… which does take a while longer than the actual
birth part. She talked about her
skiing vacation and other things.
She said everything looked good.
Then she told me, “Because you have high blood pressure, we’re going to
put you on magnesium fluids for 24-36 hours. Magnesium is a preventative that will stop you from having
any seizures or strokes.”
It’s nasty stuff, all that fluid. The doctor also warned me that magnesium would make me very
bloated and very sleepy. She was
right on both those aspects and both of those things later contributed to some
negative baby blue issues.
When the doctor was finished stitching me up, the nurses told
me that they would move me to another bed. Fortunately they warned me first with these words, “It’s
going to feel weird. It’s going to
feel like you are going to fall off of the bed, but trust us, we have you. You won’t fall.” I’m glad for the warning, because I
would have freaked out otherwise.
For the first 36 hours of our son’s birth, I was not fully
aware of what all was going on, because I was being given percocet and motrim
around the clock for pain, along with the magnesium and additional fluids. My blood pressure was being monitored
as well as kidney functions, once both were confirmed to be stable, after the
36 hours, then I was taken off of the magnesium and catheter.
But during those 36 hours? My husband was incredibly happy, holding the baby and
changing diapers, etc. For me, I
had lactation nurses come in, asking, “How are your nipples today?” Of which my husband laughed and said,
“Not something you usually get away with asking!” Unfortunately, because of a c-section and magnesium and
fluids and hypothyroidism, my milk was slow to start.
But not for the lactation nurses trying… good grief, I saw
at least 10 different lactation nurses and it HURT having someone pinch and
squeeze you like that over and over again. My breast did manage to produce some colostrums, which is very
important for a new born, so at least that happened. But as our son’s weight went from 6.12 to 6.5, the nurses
suggested formula feeding and to use a breast pump in the meantime.
It was disheartening.
And while I was being shown how to pump, my husband was given
instructions on bottling feeding our baby. Again, this made for some baby blue issues to work through
when we got home.
When I was on the magnesium, the nurses would come in and
press hard on my stomach to make sure the uterus was going back down. Want to know what pain is? Yeah, when you are so drugged up with 3
different pain medicines and STILL feel pain, that’s pain. So much so that I was gripping my hands
into the side of the bed from stopping myself from hitting the nurse kind of
pain.
Oh and when they have to “check the blood flow” –
embarrassing… They are looking at the pad and when you still have a catheter in
and they move the pad – that hurts!
It was a relief to get the catheter out, but warning, when the nurse
tells you, “I’m going to count to three and on three, I want you to take a deep
breath” – do as she says, the deep breath helps with removing the catheter.
The recovery nurses up to this point were very caring and
attentive, but then we were moved to the post partum room, which was much
smaller and the nurses not only had the post partum maternity, but also any
surgeries in recovery to take care of.
Needless to say, too many patients and not enough staff leads to not as
solid care, but what can be expected with budget cuts?
Before we left the hospital, one of the nurses was very
helpful in saying, “These are the things you paid for with the hospital bill,
take them home.” That included the
formula, Johnson&Johnson bath supply, nasal thingie, breast pump pieces (insurance
paid for the pieces because it was a medical need as our son did not latch),
diapers, etc. It was helpful to
bring these things home, even though we had a starter with a lot of products
from the baby shower. It was still
good to have the formula, to know what our son was used to and hospital
approved.
People think that c-sections are great, because you don’t
have labor pains (if it’s scheduled and you don’t induce first), but they
forget that this is major surgery and the recovery is a lot harsher on the body
than natural delivery. I wasn’t
able to get out of bed until we were in post partum and when I stood up, it was
more like the hunchback. It took
all of my energy just to stand up straight and my gosh, it hurt like you wouldn’t
believe. I wondered if I would
walk straight up again! Greg was
on one side helping me and the nurse on the other and I had to take the
smallest baby steps ever just to get to the bathroom. Walking the shortest distance in the room was a huge milestone
for me and I was still on pain medicine at the time. Crazy insane to think c-sections are easier. I don’t recommend it unless it’s a
medical reason.
It’s two weeks and a few days since the surgery and I still
feel the pain in my stomach and my back. I’m not on pain medicine though. I tried to get off of those two prescriptions as soon as I
could, because people get hooked on that stuff. But I will admit, I probably tried to get off of the pain
medicine too soon. I think I could
have handled the baby blues a lot better if the pain wasn’t so bad and the
medicine does help you to sleep… and I know I was sleep deprived (still am
unless family members take a night shift to help). So, if someone would ask, I’d tell them to take the pain
medicine at least the first week home and decrease what you use for the second
week. I wish I had done that and
maybe the baby blues would have been a little more on the foggy side.
Not being able to drive for 3 weeks stinks. Total recovery is a minimum of 6 weeks
before normal activity. Not
supposed to lift anything more than 10 pounds in the meantime. You still have to deal with bleeding
with a c-section. Supposed to feed
a baby 8 times a day and pump and stay functional. Lots of changes in life and all while trying to
recover. No, I’d say go natural if
possible. My doctor did a great
job with the surgery and she even called me one night at 7:30pm to see how I
was doing and recommended anti-depressants (which I didn’t take) for the baby
blues.
I sound like it’s all complaining towards the end, but the
recover is the worst and I’m still in the middle of it. So, that’s the end of this
perspective. I’m sure there’s a
silver lining in the distance.
Family support has been so incredibly important and appreciated. Once our baby starts to sleep more
hours, it will be another blessing to count. My husband is overjoyed about being a Daddy. Though I do have to admit that I crave
and cry for our alone time and snuggle time. I’m sure the future will find a way for that as well.
So, that’s my honest review of the c-section. The surgery isn’t the scary part. If you know you’re going to have
surgery, get your family and friends lined up to help you for recovery. Never, never turn away help with a new born baby. Know that you might miss out on some
things depending on what type of medicine you need, just be prepared for it
emotionally and accept that with time the body heals.
That’s the best advice I can offer. I know it seems that I’m being
incredibly negative about the experience.
But I’d rather be honest.
For the purpose that if a woman who is about to have a c-section reads
this and has similar reasons for the c-section, then she can be better equipped
physically and emotionally for what she might experience.
All that said… I wouldn’t change doing the c-section. It was the healthiest option for our
son’s birth. We made a good call
in doing so for his well-being.
Our son is healthy and beautiful and it was worth whatever recovery and
baby blues brings. I think that’s
the strength of a parent’s love.



Comments
That magnesium is nothing nice! I got mine almost immediately after I was admitted. You're not allowed to eat for 24 hours, but somehow they tried to make an exception. That was not a good idea, because mag cause nausea. I can only imagine how hungry you must have been after having to fast for the surgery.
I actually figured it out and my sister had her c-section a couple days earlier in her pregnancy. (they were trying to do a version for breech) They didn't even try the version until 37 weeks when a baby is considered full term.
I know from the experiences of several women close to me that C-sections suck. But as you acknowledged, it was the only way. It must be very hard to be recovering from a major operation (yes, MAJOR) and nurturing a child. Thanks for your strenth, and thanks to those who love you for supporting you!